Nipple blanching (turning white) after a feeding occurs when the blood flow to the nipple is limited or cut off. Blanching is most often related to latch problems. Nipple blanching is often, but not always, associated with pain. Because women may describe shooting, burning breast/nipple pain, this can be mistakenly diagnosed as thrush. If the normal color returns after your baby has finished a feeding and there is no pain, then the blanching is not a problem.
Blanching due to compression
The most common reason for nipple blanching is that that baby is compressing the nipple while nursing. This can be due to:
Now infants can get
all their vitamin D
from their mothers’ milk;
no drops needed with
our sponsor's
TheraNatal Lactation Complete
by THERALOGIX. Use PRC code “KELLY” for a special discount!
- a shallow latch (the most common problem)
- improper sucking
- baby clamping down to slow a too-fast let-down
- tongue-tie
- baby clamping due to allergies
- clampdown bite reflex
- palate variations, etc.
When blanching is due to baby’s compression of the nipple, the nipple is white and often misformed (flattened, creased, pointed, etc.) immediately upon coming out of baby’s mouth. There may be a white stripe across the nipple directly after nursing. Pain may not start until a few seconds to a few minutes after nursing, as the circulation returns to the nipple. If you are experiencing pain with the blanching, then finding and remedying the underlying cause will also eliminate the blanching.
Blanching due to vasospasm
Vasospasm, which is more severe, is a sudden constriction/narrowing of a blood vessel (in the nipple, in this case) that is extremely painful. It might occur a short time after nursing or in between nursings. Vasospasm can have various causes:
Vasospasm can be a secondary response to pain or nipple trauma (damaged nipples or thrush). In this case, the nipple(s) turns white shortly after nursing (rather than coming out of baby’s mouth white and misformed). Mom might notice a white circle on the face of the nipple a few seconds to a few minutes after breastfeeding. Cold often triggers the vasospasm and/or makes it worse. Unlike blanching due to compression, latch and positioning may be fine if the source of any nipple damage has already been fixed. Healing the nipple trauma or other source of pain should eliminate the vasospasms, although they may persist for a short time after the nipple has healed (previously damaged tissue can remain sensitive for a time).
Raynaud’s of the nipple
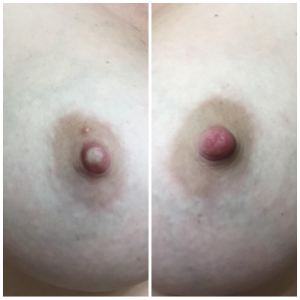
White and red phases of vasospasm from Raynauld’s. Image used with permission.
Vasospasm can also be caused by Raynaud’s Phenomenon (more info here), which causes sudden vasospasms in the extremities. When nipple vasospasm is caused by Raynaud’s Phenomenon (Raynaud’s of the nipple), the nipple turns white, then there is usually a noticeable triphasic color change – from white to blue to red – as blood flow returns. The color change may also be biphasic – from white to blue.
Vasospasm due to Raynaud’s is more likely to occur on both sides (rather than just one nipple), lasts for relatively long periods of time (rather than for a few seconds or a few minutes), and can occur during pregnancy and/or at times unrelated to feeding. Vasospasms may also occur in fingers or toes. Cold typically triggers the vasospasm and/or makes it worse. Nipple trauma (and other causes of compression blanching or vasospasm) can exacerbate the problem. Raynaud’s phenomenon may recur with subsequent pregnancies/breastfeeding, so be prepared to seek treatment quickly if you have experienced this in the past.
Per Anderson et al, “Because the breast pain associated with Raynaud’s phenomenon is so severe and throbbing, it is often mistaken for Candida albicans [yeast] infection. It is not unusual for mothers who have Raynaud’s phenomenon of the nipple to be treated inappropriately and often repeatedly for C albicans infections with topical or systemic antifungal agents.”
Keep in mind that Raynaud’s is not caused by breastfeeding (anyone might have it) — it simply has the potential to affect breastfeeding. For example, any person might have inverted nipples, which might or might not affect a mother’s breastfeeding relationship (as this can make latching or sore nipples more of a challenge in the beginning). Raynaud’s works the same way – anyone might have it coming into breastfeeding, and it might (or might not) affect the breastfeeding relationship if the vasospasms are triggered by bad latch, a sudden temperature change as baby unlatches, etc.
Some maternal medications have been associated with vasospasm, including oral contraceptives containing estrogen. Fibromyalgia, rheumatologic diseases (eg, systemic lupus erythematosus or rheumatoid arthritis), endocrine diseases (eg, hypothyroidism or carcinoid), and prior breast surgery have also been associated with Raynaud’s phenomenon. Some sources indicate that the antifungal medication fluconazole may be associated with vasospasm, although the manufacturer does not report this as a known complication of fluconazole use. Other sources feel that vasospasms experienced by mothers taking fluconazole are a result of nipple pain/trauma due to thrush (and not due to the medication used to treat the thrush).
Treatment options for vasospasm
- Avoid cold. Apply dry heat to the breast when needed (this relaxes the “cramping” blood vessels). Some mothers benefit from keeping the entire body warm (warm clothing, warm room, wrap up in a blanket, etc.)
- Cover the nipple as soon as possible after baby comes off the breast. Some moms say that it is helpful use a wool breast pad or a soft cloth diaper.
- Apply dry heat immediately after breastfeeding. A rice sock can be useful as a source of dry heat: Fill a sock or a cloth bag with uncooked rice and microwave 45 seconds (or until desired warmth is achieved); hold the rice sock against the nipple (over the cloth or mom’s shirt) until blood flow resumes.
- Massage the nipple with olive oil when mom is feeling pain from the vasospasm.
- Avoid caffeine, nicotine/smoking, diet pills, cold medications containing pseudoephedrine or phenylephrine, beta blockers, and other vasoconstrictive drugs, as they can precipitate symptoms. Oral contraceptives containing estrogen have also been associated with vasospasm.
- Medications and dietary supplements may also be helpful:
- Ibuprofen.
- Dietary supplementation with calcium/magnesium.
- Dietary supplementation with a vitamin B complex that includes B6 and niacin.
- Dietary supplementation with fish oil supplements.
- Low dose oral nifedipine.
See links below for additional details.
Additional information and references
Nipple pain – links @ ![]()
Vasospasm and Raynaud’s Phenomenon by Jack Newman, MD
Nipple Vasospasm and Breastfeeding by Philippa Pearson-Glaze IBCLC
Patient information: Raynaud phenomenon (Beyond the Basics) by Fredrick M Wigley, MD
Clampdown Bite Reflex by Mary Jozwiak, from Leaven, Vol. 30 No. 4, July-August 1994, pp. 53-4.
References
Anderson JE, Held N, Wright K. Raynaud’s Phenomenon of the Nipple: A Treatable Cause of Painful Breastfeeding. Pediatrics. 2004 Apr;113(4):e360-4.
Garrison CP. Nipple vasospasms, Raynaud’s syndrome, and nifedipine (case report). J Hum Lact. 2002 Nov;18(4):382-5.
Riordan J and Auerbach K. Breastfeeding and Human Lactation, 2nd ed. Boston and London: Jones and Bartlett 1999, p. 492-493.
Lawlor-Smith L, Lawlor-Smith C. Raynaud’s phenomenon of the nipple: a preventable cause of breastfeeding failure? Med J Aust. 1997 Apr 21;166(8):448.
Lawlor-Smith L, Lawlor-Smith C. Vasospasm of the nipple – a manifestation of Raynaud’s phenomenon: case reports. BMJ. 1997 Mar 1;314(7081):644-5.
Snyder JB. [letter]. J Hum Lact. 1994 Sept;10(3):153.
Escott R. Vasospasm of the nipple: another case [letter]. J Hum Lact. 1994 Mar;10(1):6.
Coates MM. Nipple pain related to vasospasm in the nipple? J Hum Lact. 1992 Sep;8(3):153.
An Overview of Solutions to Breastfeeding and Sucking Problems by Susan Meintz Maher, IBCLC, La Leche League 1988, p 14.
