Breastfeeding my Type 1 Diabetic Baby
I was three years old when my sister was born. I don’t have many memories of myself at that age, but I do know that I was excited that there was going to be a baby. I could not wait to be a “Little Mommy” to a real, pinky, squishy infant. To help me feel part of the process, my parents bought me a baby doll, whom I named Sarah. I can still smell the powder-fresh, newborn-scented plastic. That doll went everywhere with me for years. I changed her, bathed her, and dressed her, just like my mom did with my baby sister. I even sat in my chair, delicately lifted my Little Mermaid t-shirt, and nursed my Sarah doll.

Nursing my baby boy then and now.
Now infants can get
all their vitamin D
from their mothers’ milk;
no drops needed with
our sponsor's
TheraNatal Lactation Complete
by THERALOGIX. Use PRC code “KELLY” for a special discount!

Siblings bond over tandem nursing.

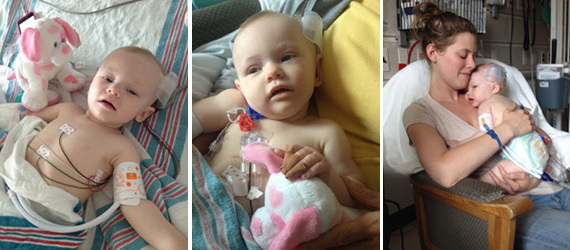
The day before Baby Girl's diagnosis. She just wasn't herself.
When the office opened, I called to make the appointment and started getting ready. She had been so fussy and just wanted to be held. I stepped away from her crib to quickly change. When I came back, I knew in my heart that something was horribly wrong. Her rosy, pink cheeks were sunken deep and her bright eyes were dark and unresponsive. Then, I noticed her breaths were deep and labored, exposing her delicate skeletal frame beneath her sleeper. At this point, I was terrified to put her in the car for fear that she would fall asleep and never wake up.

Just before calling the ambulance--the picture I texted my husband while he was at work.
At the emergency room, it took under five minutes for our baby girl to be given a diagnosis of the auto-immune disease, type-one diabetes. I agonized as I quickly asked the attending ER doctor if it was our fault, but I knew that it wasn’t. My daughter was still basically exclusively breastfed, as she really wasn’t interested in solids yet and there is no known cause to this chronic medical condition. Once she had a central line put in and IV fluids were started, I asked when I could nurse her. I didn’t get a straight answer and I felt paralyzed with fear as I flashed back to our last nursing session. It was hurried. I was trying to get her to breastfeed before we left for the doctor’s office, but she really wasn’t interested. She was so unaware of her surroundings at the time and I remember being concerned. It was at that point that I thought, “What if that was the last time I will ever nurse her again?” I knew that diabetes required careful attention to what was consumed. What if they made me switch to formula so we could accurately count the carbs my daughter would consume? What if I had to become an exclusive pumper so they could track how many ounces she drank? I tried to push the thought out of my head. We had only just arrived at the hospital and they were transferring us to the pediatric intensive care unit. I would find out there. I settled on asking for a pump. I was so engorged from our shortened earlier nursing and I made up my mind to have milk ready for her when the time came. I had to keep stimulating to make sure I had milk when she was ready for it.
 It wasn’t until we got to the PICU that I realized just how serious things were and how close we were to losing our little girl. It was surreal listening to the attending physician ask questions of the medical students and discuss her treatment. For the first time that day, I was truly scared that she might not make it. She was in diabetic ketoacidosis and her blood sugar was in the 600’s. Her electrolytes were all out of whack and she was lethargic and mostly unresponsive. I also quickly learned that once her levels were stabilized, managing her new medical condition would be much more difficult than I had originally anticipated. I emphatically told our nurse that our daughter was exclusively breastfed. She told me that for now, she was getting what she needed through her IV. I asked if and when I would ever be able to nurse again. My heart sank when she said she didn’t know, but that she would find out. I prepared myself for the worst and began to mourn the loss of nursing my baby girl. I felt a twinge of guilt for feeling so defeated. She was alive, after all, but one of the most important parts of our current relationship was being threatened and was on the verge of extinction. I was devastated.
It wasn’t until we got to the PICU that I realized just how serious things were and how close we were to losing our little girl. It was surreal listening to the attending physician ask questions of the medical students and discuss her treatment. For the first time that day, I was truly scared that she might not make it. She was in diabetic ketoacidosis and her blood sugar was in the 600’s. Her electrolytes were all out of whack and she was lethargic and mostly unresponsive. I also quickly learned that once her levels were stabilized, managing her new medical condition would be much more difficult than I had originally anticipated. I emphatically told our nurse that our daughter was exclusively breastfed. She told me that for now, she was getting what she needed through her IV. I asked if and when I would ever be able to nurse again. My heart sank when she said she didn’t know, but that she would find out. I prepared myself for the worst and began to mourn the loss of nursing my baby girl. I felt a twinge of guilt for feeling so defeated. She was alive, after all, but one of the most important parts of our current relationship was being threatened and was on the verge of extinction. I was devastated.
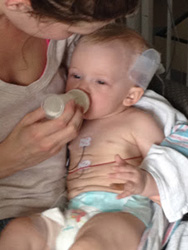
First bottle of pumped breast milk.

First latch after receiving her insulin pump. I don't know who was happier!
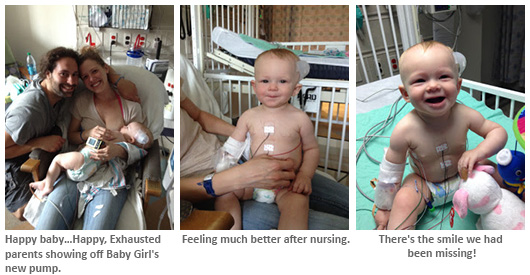

Packing up to head home!

Signs and Symptoms of Type 1 Diabetes include excessive thirst, excessive urination, weight loss, and extreme hunger. If breath smells fruity, there is vomiting, and/or deep, rapid breathing, head to emergency immediately! With our daughter, I mistakenly thought the leaks in her cloth diapers were because I was washing them incorrectly or putting them on her the wrong way. In hindsight, she was wetting through them quickly because of her high blood sugars! The first sign we saw was the vomiting, which we attributed to a stomach bug that had been going around. It is so difficult to diagnose babies with Type 1. You know your child best. If he or she is “just not acting him/herself”, seek medical attention. We have set up a non-profit to raise awareness for Type 1. Check out www.facebook.com/jamforjoyt1d. For more information about Type 1 Diabetes, visit www.jdrf.org.
Brittany is a wife to Nathan (July 2010) and mother to Aaron (August 2011) and Norah (August 2013). She and her family stick together, no matter how busy life gets, whether she and her husband are performing in their country/crossover band, Amanda Jones and the Family Band, or leading worship with their traveling ministry team, Imago Dei. Brittany blogs at mompodgeblog.wordpress.com covering topics of faith, family, life with a newly diagnosed type 1 baby, and her transition to living more naturally and sustainably.
All images are the property of the author. Do not use without permission.
More
Breastfeeding the Type 1 Diabetic Child @ KellyMom
