
Image credit: RaphaelGoetter on flickr
Milk production begins around the midpoint of pregnancy. For most mothers, milk will “come in” (increase in quantity and begin the change from colostrum to mature milk) between days 2 and 5.
Is there milk in my breasts at birth?
Yes! Colostrum is being produced from about 16-22 weeks of pregnancy, although many mothers are not aware that the milk is there since it may not be leaking or easy to express. Colostrum is the early, concentrated milk that is full of nutrients and disease-fighting antibodies — it provides everything that your baby needs in the early days after birth. Your baby’s stomach is very small at birth, and the amounts of colostrum (transitioning gradually to mature breastmilk once your milk comes in) are perfect for baby’s needs. The average colostrum intake by healthy babies increases from 2-10 mL per feeding in the first 24 hours to 30-60 mL (1-2 oz) per feed by the end of day 3 (ABM 2009).
Now infants can get
all their vitamin D
from their mothers’ milk;
no drops needed with
our sponsor's
TheraNatal Lactation Complete
by THERALOGIX. Use PRC code “KELLY” for a special discount!
Average Intake of Colostrum/Milk
| Baby’s Age | Per Feeding | Per 24 hours |
| Day 1 (0-24 hours) | 2-10 mL (<½– 2 tsp) | 30 mL (1 oz) |
| Day 2 (24-48 hours) | 5-15 mL (1 tsp – ½ oz) | |
| Day 3 (48-72 hours) | 15-30 mL (½– 1 oz) | |
| by Day 7 | 30-60 mL (1-2 oz) | 300-600 mL (10-20 oz) |
| Weeks 2 & 3 | 60-90 mL (2-3 oz) | 450-750 mL (15-25 oz) |
| 1-6 months | 90-120 mL (3-4 oz) | 750-1035 mL (25-35 oz) |
References: ABM 2009, Mannel et al 2013, Mohrbacher 2010.
When can I expect my milk to increase?
Milk production normally begins to increase (biochemically) between 30 and 40 hours after delivery of the placenta, but it may take a little while for the changes to become apparent to the mother. Milk “coming in” generally refers to the time when the mother notices increased breast fullness (and other signs) as milk production begins to kick into full gear– this usually occurs 2-3 days after birth, but in as many as 25% of mothers this may take longer than 3 days.
Signs that your milk is increasing may include:
- breast fullness, swelling, heaviness, warmth, engorgement, tingling
- leaking milk
- change in baby’s feeding patterns and behavior at the breast
- if you’re expressing milk or leaking, you may notice the milk begin its gradual change in appearance from the thicker golden colostrum to the thinner, whiter mature milk
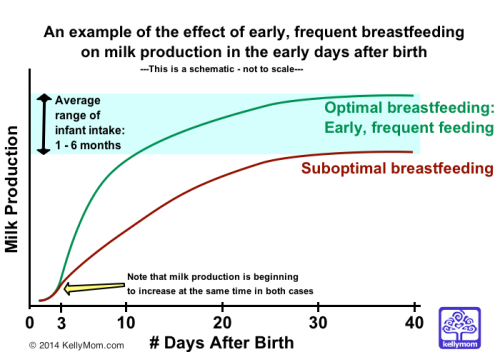
Keep in mind that many women experience their milk coming in as a gradual change, rather than a sudden one. Research indicates that this timing is hormonally controlled – it does not require that baby be breastfeeding at all. However, mothers who breastfeed early and often (or express milk if breastfeeding is not going well) have higher milk production on days 3-4, and their infants lose less weight and have lower bilirubin levels (less jaundice). Skin-to-skin contact with baby has also been associated with increased milk production. Milk production will begin to shut down if milk is not being removed by the time your milk is coming in.
Risk factors for delayed onset of lactation
When a mother’s milk does not undergo the expected increase in volume within 3 days of birth (72 hours postpartum) – this is called delayed onset of lactation (DOL).
Studies have shown that risk factors for delayed onset of lactation include:
- First time mothers – tend to have milk come in about a day later than mothers with more than one child.
- Labor & Delivery factors
- Large amounts of IV fluid during labor
- Pain medications during labor, regardless of delivery method
- Stressful, exhausting, or traumatic vaginal birth
- Cesarean section (it is unclear whether this is due to the stress of surgery, medications, delaying breastfeeding, and/or less than optimal breastfeeding management)
- A long pushing stage during birth (over one hour)
- Blood loss (more than 500 mL/1 pint)
- Retained placenta or anything that affects placental function. If there is a retained placenta, the milk will typically come in normally once the placental fragments are removed.
- Maternal Health
- Issues that affect mom’s hormones or her response to hormones, including insulin resistance, unstable or poorly controlled Type-1 diabetes, polycystic ovarian syndrome, infertility, hypothyroidism or pituitary issues including Sheehan’s Syndrome, hypertension, gestational ovarian theca lutein cysts.
- Obesity
- Research suggests that instead of a true DOL, the increased risk may be due to a slower increase in production because of less than optimal breastfeeding management, a decreased prolactin response to breastfeeding, or increased body mass affecting breast development during puberty.
- In the following factors, the milk is most likely coming in on schedule, but milk production may not increase enough to be felt as increased fullness
- Maternal breast issues
- Preterm birth (may cut short the breast growth of late pregnancy, resulting in less milk producing tissue at birth, but good breastfeeding management will result in breast growth continuing after birth)
- Underdeveloped breasts – Hypoplasia/Insufficient Glandular Tissue
- Breast surgery or injury (may either remove/damage breast tissue or damage nerves that interfere with milk ejection)
- Unusual nipple anatomy, flat or inverted nipples, or nipple piercing have the potential to interfere with milk transfer
- Any breastfeeding management issue, including maternal illness, that affects milk removal from the breast in the early days
- Any medication that decreases milk production in the early days, including hormonal birth control.
- Maternal breast issues
What do I do if my milk does not come in by day 4?
- Optimize breastfeeding management to make sure the breast is being emptied frequently and thoroughly; skin-to-skin contact with baby can also help with milk production.
- Monitor baby’s weight to make sure he/she is getting enough milk – if your baby loses more than 7% of birth weight, breastfeeding should be evaluated. If baby is not getting enough milk, supplementation may be warranted.
- Schedule a visit with a local board-certified lactation consultant to make a plan to increase your milk production and monitor baby’s progress.
- If a cause can be determined for the delay, there may be further measures that you can take to remedy the situation (for example, if retained placental fragments are the issue, the milk usually comes in normally once the placental fragments are removed). Checking endocrine levels (thyroid, testosterone, prolactin) may be useful.
- If you’re struggling after a difficult start: Remember that many mothers have been able to slowly bring in a full milk supply after a week or two (and sometimes even after many weeks!).
References and more information:
Breastfeeding your newborn — what to expect in the early weeks @KellyMom.com
Increasing Low Milk Supply @KellyMom.com
How Does Milk Production Work? @KellyMom.com
ABM [Academy of Breastfeeding Medicine] Clinical Protocol #3: Hospital guidelines for the use of supplementary feedings in the healthy term breastfed neonate, revised 2009. Breastfeed Med. 2009;4(3):175-82.
Chapman DJ, Pérez-escamilla R. Maternal perception of the onset of lactation is a valid, public health indicator of lactogenesis stage II. J Nutr. 2000;130(12):2972-80.
Hurst NM. Recognizing and treating delayed or failed lactogenesis II. J Midwifery Womens Health. 2007;52(6):588-94.
Lawrence RA, Lawrence RM. Breastfeeding, A Guide for the Medical Profession (7th ed.). Elsevier Health Sciences; 2011; 81, 84-85, 552.
Lind JN, Perrine CG, Li R. Relationship between Use of Labor Pain Medications and Delayed Onset of Lactation. J Hum Lact. 2014;30(2):167-73.
Mannel R, Martens PJ, Walker M. Core Curriculum for Lactation Consultant Practice (3rd ed.). Jones & Bartlett Publishers; 2013; 289-291, 356, 594, 818.
Mohrbacher N. Breastfeeding Answers Made Simple, A Guide for Helping Mothers. Hale Pub L P; 2010; 63, 70-74, 109, 409-413.
Riordan J, Wambach K. Breastfeeding and Human Lactation (4th ed.). Jones and Bartlett Publishers; 2010; 267, 330-337, 346-347.
