By Kelly Bonyata, BS, IBCLC To understand how to … [Read more...]
Archives for August 2011
Tips for juggling a newborn and toddler
(not literally... well, usually not literally!) First off, … [Read more...]
Foremilk and hindmilk – what does this mean?
By Kelly Bonyata, BS, IBCLC Normally the changing fat … [Read more...]
Lactation yoga …side-lying nursing without getting up to switch sides
...or side-lying nursing without getting up to … [Read more...]
Establishing and maintaining milk supply when baby is not breastfeeding
By Kelly Bonyata, BS, IBCLC It is important to express … [Read more...]
Latching: Thoughts on pushing baby’s chin down when latching
When it comes to pushing down on baby's chin to get a wider … [Read more...]
Relactation and Adoptive Breastfeeding: The Basics
By Kelly Bonyata, BS, IBCLC Relactation or induced … [Read more...]
Breastfeeding Logs
By Kelly Bonyata, BS, IBCLC Under normal circumstances it is … [Read more...]
Breastfeeding Helplines
International International Lactation Consultant Association … [Read more...]
Weaning from formula supplements
Put baby to breast often Aim for 10 breastfeeding sessons … [Read more...]
Growth spurts
Most babies go through several growth spurts (also called … [Read more...]
Cluster Feeding and Fussy Evenings
By Kelly Bonyata, BS, IBCLC It is very common for babies to … [Read more...]
The Distractible Baby
By Kelly Bonyata, BS, IBCLC Is my baby distractible? … [Read more...]
Reverse Cycling
By Kelly Bonyata, BS, IBCLC What is reverse … [Read more...]
Do babies under 12 months self-wean?
Deutsch By Kelly Bonyata, BS, IBCLC Introduction … [Read more...]
Breastfeeding Your Toddler: What to expect
By Kelly Bonyata, BS, IBCLC Are you considering … [Read more...]
Breastfeeding and Fertility
By Kelly Bonyata, BS, IBCLC How can I use breastfeeding … [Read more...]
Getting Pregnant While Breastfeeding
PDF version (great for printing) By Hilary Flower, author … [Read more...]
Forceful Let-down (Milk Ejection Reflex) & Oversupply
By Kelly Bonyata, BS, IBCLC Is forceful let-down the … [Read more...]
Normal prolactin levels in breastfeeding mothers
Typical baseline serum prolactin levels in … [Read more...]
Let-down Reflex: Too slow?
By Kelly Bonyata, BS, IBCLC Is my let-down functioning … [Read more...]
Breastfeeding in Public
Commentary Links More commentaries on … [Read more...]
Breastfeeding: Legal Issues
Do you need information on legal issues and breastfeeding? … [Read more...]
Jury Duty?
A call to jury duty can be very worrisome for mothers who … [Read more...]
Breastfeeding & Jury Duty – My Experience
by Jeni Panhorst. Reprinted with permission from the … [Read more...]
Breastfeeding and Speech Development
Breastfeeding... Promotes normal oral-facial … [Read more...]
Average Weight Gain for Breastfed Babies
Average weight gain Average length & head … [Read more...]
Average Weight Gain for Breastfed Babies (Metric)
[click here for English Units (ounces/inches) and … [Read more...]
Average Toddler Growth
Some things to look at to determine that your child is … [Read more...]
My breasts feel empty! Has my milk supply decreased?
By Kelly Bonyata, BS, IBCLC It is normal for a mother's … [Read more...]
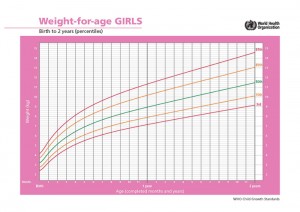
Average Growth Patterns of Breastfed Babies
By Kelly Bonyata, BS, IBCLC Growth charts and breastfed … [Read more...]
Is my older baby getting enough milk?
By Kelly Bonyata, BS, IBCLC IS BABY GETTING ENOUGH? … [Read more...]
Lopsided! What can I do?
...When baby prefers one side, or when supply or breast size … [Read more...]
Books to Avoid
See the Book Reviews for more information Warning: … [Read more...]
Is my exclusively breastfed baby gaining too much weight?
By Kelly Bonyata, BS, IBCLC It is normal for breastfed … [Read more...]
Secrets of the Baby Whisperer: How to Calm, Connect, and Communicate with Your Baby
by Tracy Hogg, with Melinda Blau Ballantine Books, New … [Read more...]
Good Nights – The Happy Parents’ Guide to the Family Bed (and a Peaceful Night’s Sleep!)
by Jay Gordon, M.D. and Maria Goodavage Griffin Trade … [Read more...]
The Joyful Family – Meaningful Activities and Heartfelt Celebrations for Connecting with the Ones You Love
by John Dacey, PhD, and Lynne Weygint Conari Press, Berkely … [Read more...]
I’m Made of Mama’s Milk
written, illustrated & published by Mary Olsen ISBN: … [Read more...]
The “What to Expect” Series
The "What to Expect" Series by … [Read more...]
Mini-Reviews – Parenting & Sleep (various books)
The Mighty Toddler by Robin Barker … [Read more...]
Mini-Reviews – Nutrition (various books)
Child of Mine: Feeding With Love and Good Sense by Ellyn … [Read more...]
Stillen sich Babys unter zw�lf Monaten selbst ab?
English Deutsch von Cordula Kolarik (e-mail: … [Read more...]
Кърмене на бебе над 1 година
By Kelly Bonyata, BS, IBCLC Translation by: Анелия … [Read more...]
ФАКТЫ О ПРОДОЛЖИТЕЛЬНОМ КОРМЛЕНИИ ГРУДЬЮ
By Kelly Bonyata, BS, IBCLC Translation by: Оксаной … [Read more...]
Beneficios de la lactancia prolongada
By Kelly Bonyata, BS, IBCLC Traducción: Andrea … [Read more...]
Предно и задно мляко
By Kelly Bonyata, BS, IBCLC Translation by: Анелия Донева … [Read more...]
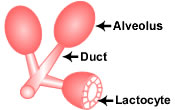
Как се образува млякото?
By Kelly Bonyata, BS, IBCLC Translation by: Анелия Донева … [Read more...]
What is a galactagogue? Do I need one?
By Kelly Bonyata, IBCLC A substance that increases milk … [Read more...]
Смягчение Давлением
By K. Jean Cotterman RNC, IBCLC Translation by: Victoria … [Read more...]
Die Ernährung gestillter Kleinkinder
English Translated and reprinted with permission from … [Read more...]
Amamantando a un bebe mayor de un año
By Kelly Bonyata, BS, IBCLC Traducción: Rosana … [Read more...]
History of Breastfeeding
OK, other that the fact that breastfeeding started with the … [Read more...]
Links: Breastfeeding Art
NOTE: Many of these images are not in the public domain. If … [Read more...]
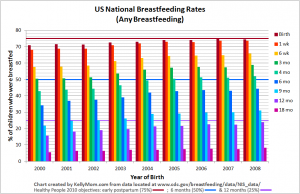
Breastfeeding: the Numbers
Breastfeeding rates in the United States and worldwide What … [Read more...]
Ross Labs breastfeeding statistics
Until relatively recently, ironically enough, the primary … [Read more...]
All I Need to Know About Life I Learned By Breastfeeding
Mammals make great mothers. … [Read more...]
Breastfeeding Quotes
"If a multinational company developed a product that was a … [Read more...]
A Father Reveals Things He Has Learned From His Children
There is no such thing as childproofing your house. A … [Read more...]
Great Truths About Life That Little Children Have Learned
No matter how hard you try, you can't baptize cats. When … [Read more...]
A Message From A Busy One Year Old
Please expect me to be busy. That is my developmental job. … [Read more...]
Toddler Property Laws
1. If I like it, it's mine. 2. If it's in my hand, it's … [Read more...]
On Starting Solids
by Eleanor Goulding Smith from The … [Read more...]
Announcing the new Toddler Miracle Diet!
Over the years you may have noticed that most 2 year olds … [Read more...]
Message From A Two Year Old
Please be glad that I'm growing up, even though I am doing … [Read more...]
Elephant Recipe
Ingredients: 1 elephant 7 bushel carrots, chopped 7 … [Read more...]
Handy Tips
Stuff your mother should have told you... If … [Read more...]
Expressions for women on high-stress days
You - Off my planet. Not the brightest crayon in the … [Read more...]
What Really Matters
A philosophy professor stood before his class and had some … [Read more...]
Women
Age 3: She looks at herself and sees a Queen. Age 8: She … [Read more...]
Mom is taking a bath
Dear Kids, Don't be alarmed; the world isn't coming to an … [Read more...]
Evolution of a Mom
Yes, parenthood changes everything. But parenthood also … [Read more...]
The First Parent
by Bill Cosby Whenever your kids are out of … [Read more...]
When God Created Moms
by Erma Bombeck see also: When … [Read more...]
Job Opening
POSITION: Parent JOB DESCRIPTION: Long term team players … [Read more...]
Just Once More
I'd like to be pregnant just once more. I'd like … [Read more...]
Laws Concerning Food and Drink; Household Principles; Lamentations of the Father
by Ian Frazier (February 1997, The Atlantic … [Read more...]
New Survivor Show
Have you heard about the next planned … [Read more...]
Parenting Quotes
"God could not be everywhere, so he created mothers." … [Read more...]
Poems and quotes on parenting
What Did I Do Today? Childhood … [Read more...]
Time for Bed
Author Unknown Mom and Dad were watching TV … [Read more...]
A substitute for natural pregnancy…
Author Unknown A substitute for natural … [Read more...]
References: Breastfeeding During Pregnancy and Tandem Breastfeeding
Recommended print resources Mohrbacher N. Breastfeeding … [Read more...]
How will breastfeeding affect my morning sickness?
There is a plus and a minus to report. First it must be said … [Read more...]
Breastfeeding during labor
Nursing naturally increases oxytocin levels, and so can … [Read more...]
How will my milk change when I am breastfeeding through pregnancy?
Milk supply during pregnancy Changes in milk composition … [Read more...]
Will tandem breastfeeding spread germs between my children?
No special measures are normally needed as far as hygiene … [Read more...]
What if I want to wean while pregnant with a new baby?
Pregnancy has a way of making moms think of weaning, … [Read more...]
Sore nipples and agitation during pregnancy
Many mothers experience nipple soreness when breastfeeding … [Read more...]
Will pregnancy cause my child to wean prematurely?
I'm committed to child-led weaning, and am worried that my … [Read more...]
How can I answer critics of tandem breastfeeding?
The first thing to bear in mind is that your breastfeeding … [Read more...]
Will I like tandem breastfeeding? Is worth the trouble?
Like everything else when a new baby first arrives, tandem … [Read more...]
How does tandem breastfeeding affect sibling rivalry?
Many tandem nursing mothers say that “reduced sibling … [Read more...]
What positions are best for tandem breastfeeding?
To find your best arrangement you will need to experiment … [Read more...]
Does my newborn always need to breastfeed first?
Although you may be advised to make sure the newborn always … [Read more...]
Nipple soreness and engorgement after birth
Breastfeeding during pregnancy and tandem … [Read more...]
Is it safe to use a breastpump during pregnancy?
It is often stated that a woman should not use a breastpump … [Read more...]
Nutrition for mom while pregnant & breastfeeding or tandem breastfeeding
Special Dietary Considerations (Nursing … [Read more...]
Will breastfeeding affect the nutrition of my unborn child?
This concern is valid for malnourished mothers, but it does … [Read more...]
Is it safe to breastfeed during pregnancy?
Yes, in most cases. At this time no medical study has been … [Read more...]
Adventures in Tandem Nursing: Table of Contents
Foreword by Peggy O'Mara Introduction PART ONE: THE … [Read more...]
Adventures in Tandem Nursing: From the back cover…
Can a mother produce enough milk for two children? How … [Read more...]
What if a “weaned” child asks to breastfeed again?
Excerpted with permission from Adventures in Tandem … [Read more...]
What if I lose weight in the first trimester (while breastfeeding and pregnant)?
Excerpted with permission from Adventures in Tandem … [Read more...]
The nature of breastfeeding contractions
Excerpted with permission from Adventures in Tandem … [Read more...]
What are miscarriage and preterm labor experts saying?
Excerpted with permission from Adventures in Tandem … [Read more...]
Pregnancy Complications while Breastfeeding
Excerpted with permission from Adventures in Tandem Nursing: … [Read more...]
Meet our new logo!
Please join me in congratulating Keith Hanssen on creating … [Read more...]
Oatmeal for increasing milk supply
By Kelly Bonyata, BS, IBCLC Eating a bowl of oatmeal, if … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Ist das Stillen während der Schwangerschaft ungefährlich?
Ja, in den meisten Fällen. Bisher sind keine klinischen … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Wirkt sich das Stillen auf die Ernährung meines ungeborenen Kindes aus?
Diese Bedenken sind bei mangelernährten Müttern angebracht, … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Ernährung der Mutter
Immer daran denken: Schwangerschaft und Stillzeit … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Ist die Verwendung einer Milchpumpe während der Schwangerschaft ungefährlich?
Es wird oft gesagt, dass Frauen in der Schwangerschaft keine … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Schmerzende Brustwarzen und geschwollenes Drüsengewebe nach der Geburt
Während der Schwangerschaft werden schmerzende Brustwarzen … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Muss das Neugeborene immer zuerst gestillt werden?
Auch wenn Ihnen dazu geraten wird, das Neugeborene immer … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Welche Positionen sind am besten für das Tandemstillen geeignet?
Um die für Sie beste Position zu finden, müssen Sie einige … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Wie wirkt sich das Tandemstillen auf die Geschwisterrivalität aus?
Viele Mütter sagen, dass eine „geringere … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Werde ich das Tandemstillen mögen? Lohnt es sich?
Wie alles andere auch nach der Geburt eines Babys wird das … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Wie kann ich auf kritische Bemerkungen reagieren?
Zunächst ist es wichtig, sich stets darauf zu besinnen, dass … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Wird sich mein Kind durch die Schwangerschaft früher abstillen?
Ich möchte, dass mein Kind bestimmt, wann es sich abstillt, … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Schmerzende Brustwarzen und Unruhe während der Schwangerschaft
Vielen Frauen tun beim Stillen während der Schwangerschaft … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Was ist, wenn ich abstillen möchte?
Eine Schwangerschaft führt auf ihre eigene Weise dazu, dass … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Werden durch das Tandemstillen Keime zwischen meinen Kindern übertragen?
Normalerweise sind keine besonderen Hygienemaßnahmen bei … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Wie verändert sich die Muttermilch?
Die Milchproduktion in der Schwangerschaft Die meisten … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Stillen unter den Wehen
Das Stillen erhöht auf natürliche Weise die … [Read more...]
Häufig gestellte Fragen zum Tandemstillen: Wie wirkt sich das Stillen auf die Schwangerschaftsübelkeit aus?
Hier gibt es gute und schlechte Nachrichten. Zuerst ist … [Read more...]
Tandem Breastfeeding: Suggestion for breastfeeding education & discussion
This exercise could be used by anyone conducting a … [Read more...]
Myths vs Facts: Breastfeeding During Pregnancy and Tandem Nursing
PDF version (great for printing) By Hilary Flower, author … [Read more...]
Breastmilk Composition
This is pretty much a list of links right now. I always have … [Read more...]
What affects the amount of fat or calories in mom’s milk?
By Kelly Bonyata, IBCLC Average calorie & fat … [Read more...]
Commentary on formulas supplemented with DHA & ARA
by Marsha Walker, RN, IBCLC. Reprinted with permission from … [Read more...]
Human milk banking and other donor milk
Informal milk sharing Milk Sharing: Formal and Informal By … [Read more...]
Formula Companies and Free Gifts
SECOND OPINION COORDINATED BY KATHLEEN RICE SIMPSON, … [Read more...]
Immune factors in human milk
In human milk, there is a complex system of antimicrobial … [Read more...]
What should I know about infant formula?
Parents consider giving their babies formula for many … [Read more...]
Calorie and fat content of various milks
Type of milk Calorie content* (kcal per ounce) Fat … [Read more...]
Is it safe to use cow’s milk or other milks as a supplement to breastfeeding?
By Kelly Bonyata, IBCLC General Guidelines Cow's … [Read more...]
Religious Fasting and Breastfeeding
By Kelly Bonyata, IBCLC Specific guidelines Jewish law … [Read more...]
Do breastfeeding mothers need extra calories or fluids?
By Kelly Bonyata, IBCLC Calories | Fluids Do breastfeeding … [Read more...]
How does a mother’s diet affect her milk?
By Kelly Bonyata, IBCLC Do I need to maintain a perfect … [Read more...]
Fenugreek Seed for Increasing Milk Supply
By Kelly Bonyata, IBCLC What is a galactagogue? Do I … [Read more...]
Can a nursing mother eat this food? FAQs
By Kelly Bonyata, IBCLC Is there a list of foods that I … [Read more...]
Herbal weight loss products and breastfeeding
By Kelly Bonyata, IBCLC Many herbal weight loss products … [Read more...]
Low carb diets and breastfeeding
By Kelly Bonyata, IBCLC High protein, low carbohydrate … [Read more...]
Can I diet while breastfeeding?
By Kelly Bonyata, IBCLC Six guidelines for safe dieting … [Read more...]
Vegetarian Diets and Breastfeeding
By Kelly Bonyata, IBCLC A vegetarian or vegan mother does … [Read more...]
Guidelines for offering juice to babies
Juice is in the same category as solid foods. Babies need … [Read more...]
Guidelines for offering water to babies
Exclusively breastfed babies do not need additional water - … [Read more...]
Finger Foods
Older babies who are just starting solids may prefer … [Read more...]
Links: Starting Solid Foods
A little humor on starting solids Starting solids What … [Read more...]
Is baby’s risk for type I diabetes increased if solids are introduced before 3 months or after 6 months?
Many parents have been concerned about the news reports … [Read more...]
How do we get started with solids?
Watch your baby, not the calendar! Should solids replace … [Read more...]
Will giving formula or solids at night help baby to sleep better?
The idea that solids will help your baby sleep is an old … [Read more...]
Is baby ready for solid foods? (Developmental signs of readiness)
What do the experts say? Health experts and breastfeeding … [Read more...]
Anemia No More
How one mother successfully battled anemia … [Read more...]
Calorie and fat content of common baby & toddler foods
Food Calorie content* (kcal per ounce) Fat content (grams … [Read more...]
Calcium
By Kelly Bonyata, IBCLC Do nursing mothers need … [Read more...]
DHA supplements for breastfeeding mothers
By Kelly Bonyata, IBCLC At present, there is a major … [Read more...]
Is Iron-Supplementation Necessary?
By Kelly Bonyata, IBCLC Why is anemia uncommon in … [Read more...]
Lecithin treatment for recurrent plugged ducts
By Kelly Bonyata, IBCLC Lecithin has been … [Read more...]
Vitamins & other supplements for breastfeeding mothers
By Kelly Bonyata, IBCLC If you eat a reasonably-well … [Read more...]
Daily Dietary Reference Intakes – Women aged 19-50
(click here for information for teens aged … [Read more...]
Daily Dietary Reference Intakes – Women (teens) aged 14-18
(click here for information for women aged … [Read more...]
Who needs vitamin B12 supplements?
By Kelly Bonyata, IBCLC Infants of well-nourished mothers … [Read more...]
There is No Doctrine for Attachment Parenting: Being AP is a Frame of Mind!
by Diana West, IBCLC Reprinted with permission from the … [Read more...]
Infant Potty Training and Attachment Parenting
by Laurie Boucke Copyright © 2003. Used with … [Read more...]
When I am a Grandmother
When I am a Grandmother When I am a … [Read more...]
Reflections…
by Paula Yount … [Read more...]
Building Your Child’s Self-Esteem
By Paul C. Holinger, M.D., M.P.H., author of What … [Read more...]
Tips for separation anxiety
by Paula Yount Mother-to-Mother.com Reprinted with … [Read more...]
Slings, wraps & other baby carriers — Why, How & Where?
Advantages of "wearing" your baby Finding a baby carrier … [Read more...]
Are you feeling overwhelmed by your child’s intense needs?
But how much intense parenting they need, possibly including … [Read more...]
Attachment Parenting Links
Articles Parenting: Day & Night (this website) What … [Read more...]
Breastfeeding & Parenting Resources for Grandparents
Your Grandchild is Breastfed? Bad News and Good News by … [Read more...]
Links: Making nursing clothing and more
Nursing Clothing | Slings | Other Nursing … [Read more...]
Links: Diaper-free babies
Infant Potty Training and Attachment Parenting by Laurie … [Read more...]
Wakeful 4 Month Olds
by Jan Barger, RN, MA, IBCLC, FILCA. Reprinted with … [Read more...]
Breastfeeding to Sleep and Other Comfort Nursing
Many mothers feel guilty for breastfeeding their baby for … [Read more...]
Co-sleeping and Bed-sharing
What is co-sleeping? Co-sleeping essentially means sleeping … [Read more...]
Got Sleep?
by Paula Yount Reprinted with permission from the … [Read more...]
Sleeping Through the Night
Should my baby be sleeping through the night? It's so common … [Read more...]
Studies on normal infant sleep
Probably one of the main reasons that babies … [Read more...]
Logo design contest entries
We've had some great entries for the logo design contest, so … [Read more...]
Gentle Discipline: Resources
Website with information and … [Read more...]
“Is it for me?” Tips for Making Your Decision about Breastfeeding during Pregnancy and Tandem Nursing
Published as “Pregnant and Tandem Nursing” by Hilary … [Read more...]
Tandem Breastfeeding: How Doulas Can Help
by Hilary Dervin Flower, MA from International Doula, Vol. … [Read more...]
How Tandem Nursing Birthed Me as a Mother of Two
by Hilary Dervin Flower Reprinted with permission from the … [Read more...]
Love, Limits and Tandem Nursing
by Hilary Flower from New Beginnings, May-June 2003, pp. … [Read more...]
Wie sicher ist das Stillen während einer Schwangerschaft?
by Hilary Dervin Flower, MA Deutsch von Utta Reich-Schottky … [Read more...]
A New Look at the Safety of Breastfeeding During Pregnancy
by Hilary Dervin Flower, MA Read article in … [Read more...]
Breastfeeding Agitation
by Hilary Flower from Leaven, Vol. 39 No. 4, … [Read more...]
Adventures in Tandem Nursing: Book Reviews
Adventures in Tandem Nursing Breastfeeding … [Read more...]
Adventures in Tandem Nursing: About the author
Hilary Dervin Flower lives in Florida with her three … [Read more...]
How Breast Milk Protects Newborns
Written by Jack Newman, MD, FRCPC Some of the molecules and … [Read more...]
Breastfeeding and Guilt
Written by Jack Newman, MD, FRCPC (revised January … [Read more...]
A Farewell to Arms – and Legs … and Feet …
excerpted with permission from: Good Nights - The Happy … [Read more...]
The Sandman Cometh: Sound Solutions for a Satisfying Sleep
excerpted with permission from: Good Nights - The Happy … [Read more...]
Good Nights – The Happy Parents’ Guide to the Family Bed: Introduction
excerpted with permission from: Good Nights - The Happy … [Read more...]
Too much milk: Sage and other herbs for decreasing milk supply
Sage This is best used only if you are in the process of … [Read more...]
Oil of Oregano for thrush?
By Kelly Bonyata, IBCLC I do not recommend … [Read more...]
Natural treatments for nursing moms
Although many medications are compatible with breastfeeding, … [Read more...]
Herbs and Breastfeeding: References
Most herbal treatments have not been thoroughly researched, … [Read more...]
Herbal safety for nursing moms
It is possible for anyone (mother or baby) to have an … [Read more...]
Breastfeeding and Thyroid Problems: Diagnostic Testing & Treatments
By Kelly Bonyata, IBCLC Thyroid screen (blood … [Read more...]
Breastfeeding and Thyroid Problems: Studies and References
(most recent listed first in each … [Read more...]
Breastfeeding and Thyroid Problems: Links
General info on thyroid problems and breastfeeding … [Read more...]
Breastfeeding and Thyroid Problems: FAQ
By Kelly Bonyata, IBCLC Is it safe for a mom with … [Read more...]
Breastfeeding and Vaccines
Vaccines in general Breastfeeding does not affect the safety … [Read more...]
Do mom’s vaccines protect her breastfed baby?
By Kelly Bonyata, IBCLC Many moms wonder whether their … [Read more...]
Conscious Sedation and Breastfeeding: Recommendations for Patients
by Maurenne Griese, RNC, BSN. Reprinted with permission from … [Read more...]
Use of Radioisotopes (and other imaging agents) during Lactation
By Kelly Bonyata, IBCLC Radiocontrast dyes … [Read more...]
Prescription drugs used for increasing milk supply
By Kelly Bonyata, IBCLC There are several prescription drugs … [Read more...]
Lactation Risk Categories
source: Medications and Mothers' Milk (2014) by Thomas W. … [Read more...]
Breastfeeding during immunizations or other painful procedures
compiled by Kelly Bonyata, IBCLC Breastfeeding during a … [Read more...]
Breastfeeding when baby has surgery
... How long before & after general anesthesia is it … [Read more...]
My baby is sick – should I continue to breastfeed?
By Kelly Bonyata, IBCLC Absolutely! Anytime a sick baby is … [Read more...]
Perchlorate in Breastmilk
by Kelly Bonyata, IBCLC There has been a large amount of … [Read more...]
PBDEs in Breastmilk
Compiled by Kelly Bonyata, IBCLC There has been a large … [Read more...]